Commercial Health Plans: Specialty Medication Management and Market Access
Highlights of the report:
Download a PDF of these Highlights
As traditional utilization management becomes well-optimized across mature and competitive specialty markets, plans are shifting toward more targeted, class-specific strategies and expanding management into the medical benefit. HIRC’s report, Commercial Health Plans: Specialty Medication Management and Market Access, explores how payers are refining their approach to specialty drug management across 14 high profile therapeutic areas. The report addresses the following questions:
- How is the regulatory environment impacting specialty drug management?
- What are commercial plans' top activities to better manage the cost and utilization of specialty drugs in 2026? Which therapeutic areas are highest priority for management?
- How are plans' utilization management tactics evolving?
- How are plans modifying their formularies for specialty drugs?
- What is the current status of biosimilars adoption and enforcement?
- What is the status of copay adjustment programs?
- What are plans top channel management and benefit alignment strategies?
Key Finding: Commercial plans are advancing utilization management towards more targeted strategies, with efforts strongly anchored in biosimilars and an increasing focus on medications covered under the medical benefit.
Formulary Management Among Plans' Leading Specialty Drug Cost Containment Strategies in 2026. Commercial health plans were asked what their organization is most focused on in 2026 to better manage the cost and utilization of specialty pharmaceuticals. Plans' activities are most often centered in formulary management, channel/site of care management and provider economics, and traditional utilization management tactics.
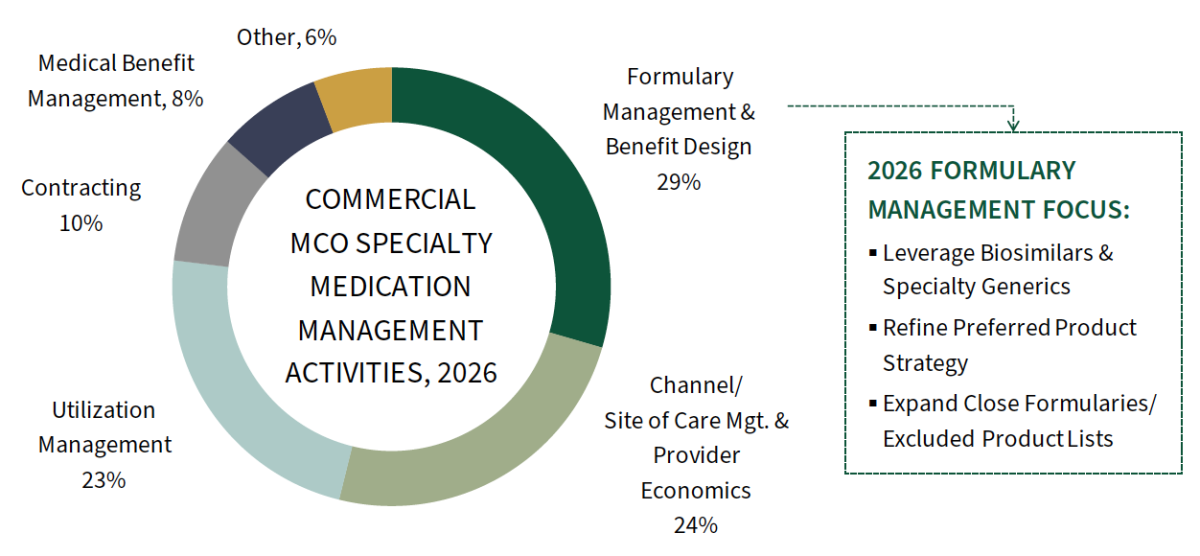
When it comes to formulary, biosimilars-first strategies are increasing as payer confidence grows and provider resistance fades. The complete report examines plans management trends across all of these topics in detail.
Biosimilars Reach a True Inflection Point. What was once a slow transition has accelerated as plans are now actively preferring biosimilars and using them as a primary lever to manage specialty spend. Plans report increased adoption of biosimilars in all categories measured, with a notable increase in adoption of STELARA and HUMIRA biosimilars over their reference brands in 2026. Commercial plans are also growing beyond new-start policies toward more active conversion in their utilization management approach.
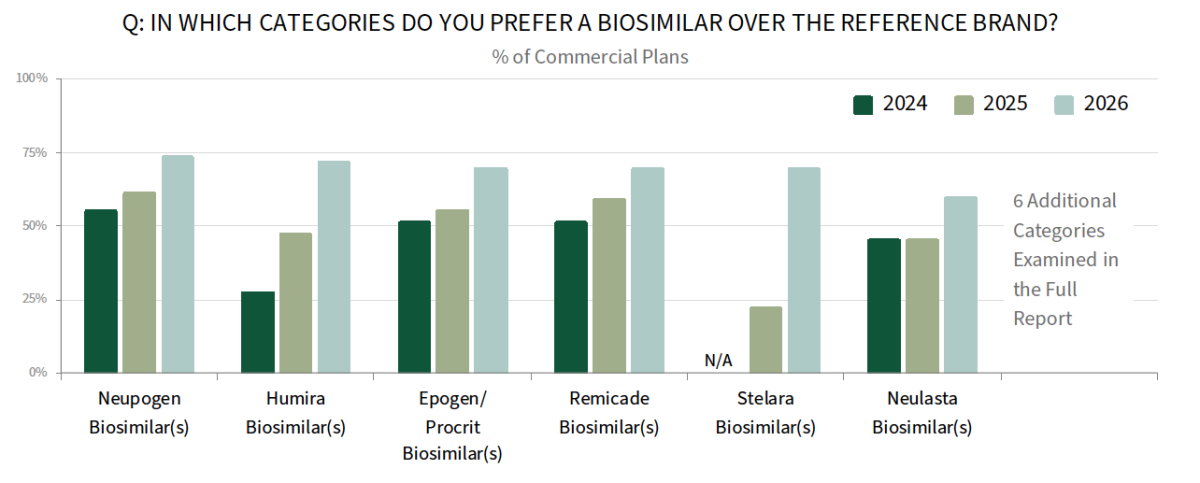
The full report examines biosimilars adoption and utilization management (UM) approaches in detail, as well as commercial plan perspectives on private-label biosimilars.
Plans Increasingly Report Medical Preferred Products. As pharmacy benefit utilization management strategies mature, plans may look to increasingly apply formulary structure and UM tools to the medical benefit, particularly for high-cost, provider-administered therapies. A higher percentage of commercial plans report preferred products on the medical benefit across many classes queried in 2026 compared to two years ago in 2024.
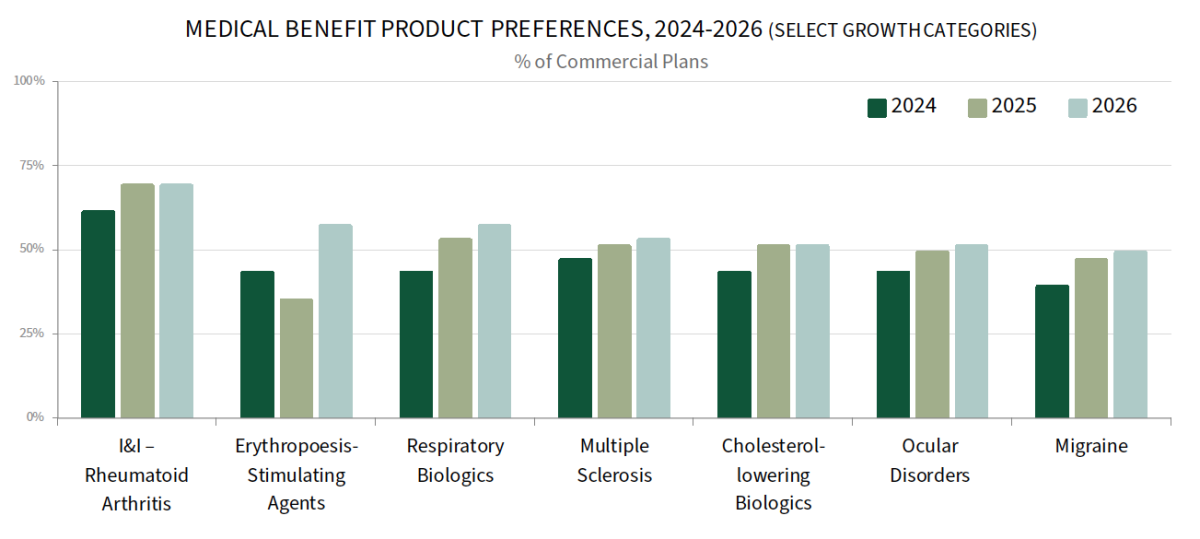
Site of care redirection and provider reimbursement are also active components of plans' medical benefit management tactics in 2026 and are examined in detail in the full report.
Research Methodology and Report Availability. In January 2026, HIRC surveyed 49 pharmacy and medical directors from national, regional, and BCBS plans representing 107 million lives. Online surveys and follow-up telephone interviews were used to gather information. The Commercial Health Plans: Specialty Medication Management and Market Access report is part of the Specialty Pharmaceuticals Service, and is now available to subscribers at www.hirc.com.
Download a PDF of these Highlights
Download Full Report (Subscribers only) >


